Overview
Approximately two per cent of Australian adults identify as lesbian, gay or bisexual. A further six to eight per cent report lifetime same-sex behaviour, and seven to fifteen per cent report same-sex attraction (source). There is a paucity of studies on rates of gender dysphoria and intersex prevalence but is estimated to be one per cent of the population for both (source 1 and 2).
The LGBTIQ acronym doesn’t refer to a homogenous group. For example, transgender, gender diverse, and intersex people can all have any sexual orientation. Lesbian, gay, bisexual, or intersex people may have fluid or transgender identities.
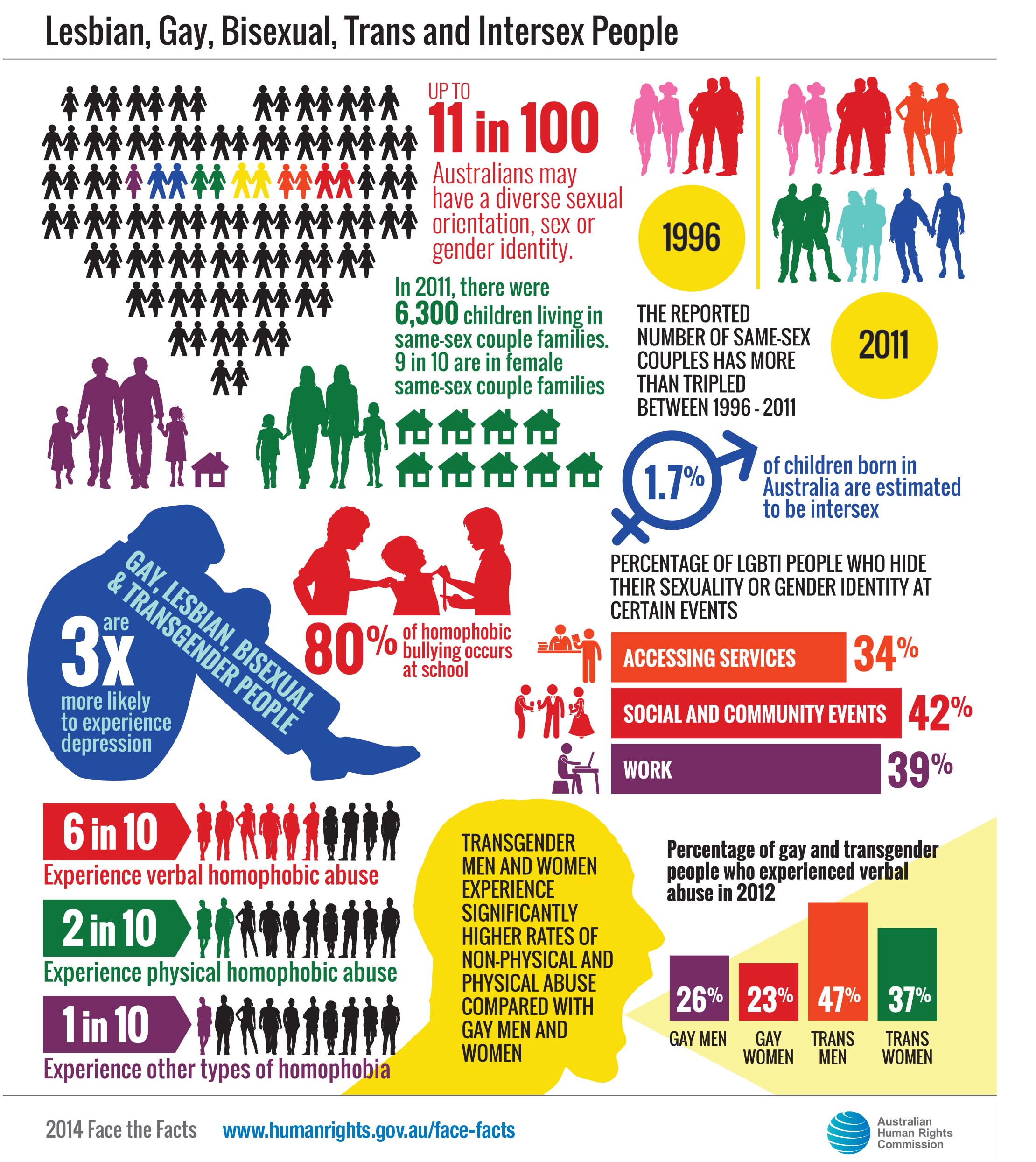
Image courtesy of the Australian Human Rights Commission.
People who identify as LGBTIQ experience significant health inequalities, which are compounded by difficulties accessing culturally sensitive health care. A systematic review of patients who identified as LGB and their experiences of health care found it to be ‘generally poor’. Major concerns included:
- Heterosexism (assumptions of heterosexuality)
- Communication barriers (for example: provider discomfort)
- Poor provider knowledge (for example: not encouraging women who have sex with women to have cervical screening tests)
- Lack of LGB-specific resources and referral networks (source)
LGBTIQ people have specific health needs including higher rates of depression, suicidal ideation, anxiety and self-harm. They are more likely to use harmful levels of alcohol and other drugs. They are also more likely to have sexually transmitted infections (STIs) and tend to delay seeking assistance with their health. LGBTIQ people are increasingly wanting to be parents and may face barriers to accessing care (source).
[accordions_pickplguins id=”14023″]
Disclaimer: This article was provided by NWMPHN. While every effort has been made to ensure the information is accurate, North Western Melbourne Primary Health Network does not warrant or represent the accuracy, currency and completeness of any information or material included within.





