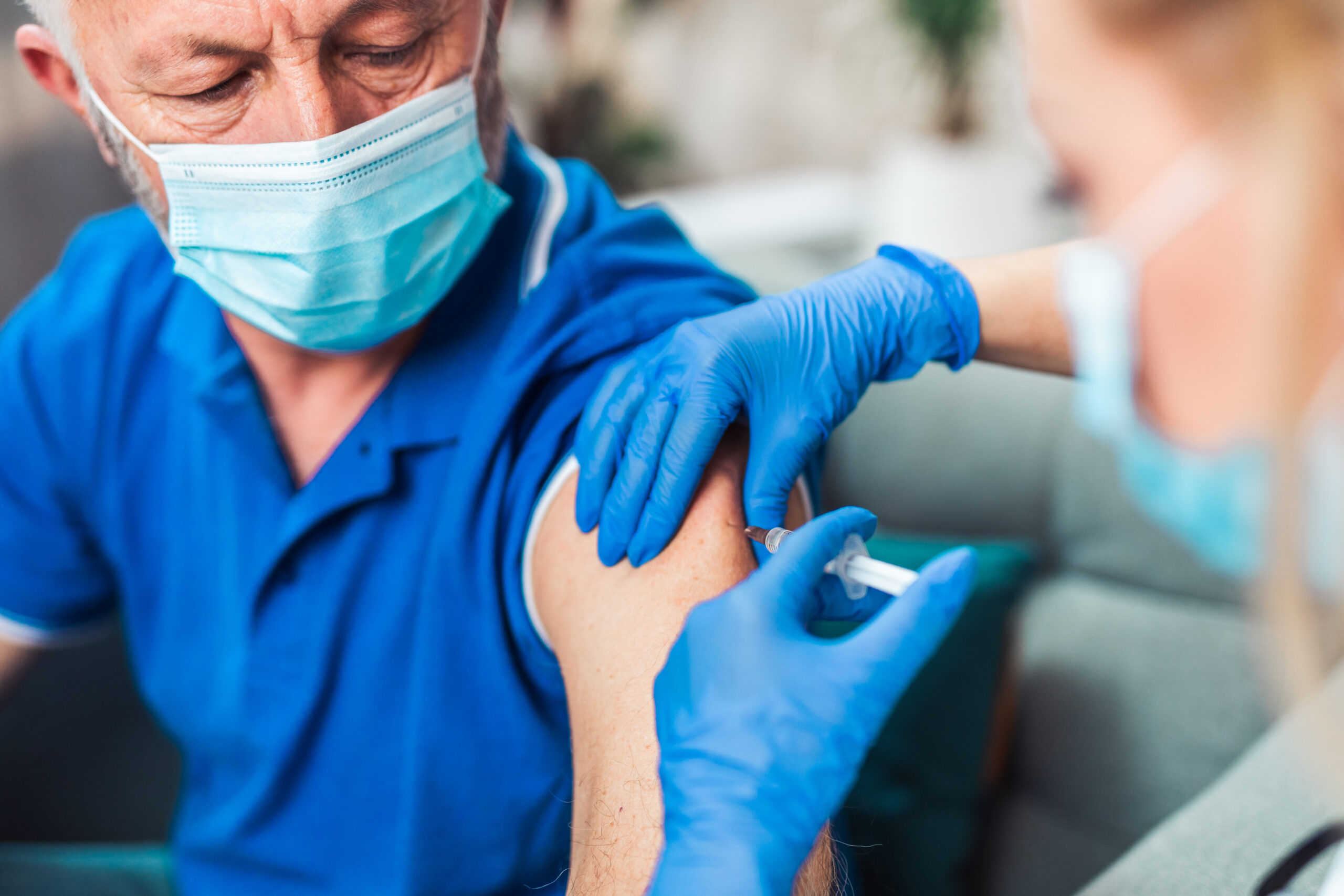
Some vulnerable groups are not getting vaccinated against COVID-19.
In the “race-not-a-race” to get everyone vaccinated, there are certain vulnerable patient groups that are less likely to be getting the jab. These include culturally and linguistically diverse (CALD) communities, low socioeconomic households and the housebound. GPs are in a unique position to assist this last group.
Am I allowed to do a COVID-19 vaccination in a patient’s home?
The Department of Health supports the off-site delivery of vaccines, including to vulnerable populations. This includes pop-up clinics, drive-through clinics, in-reach/out-reach clinics, as well as vaccinations conducted in a person’s place of residence – which may be their home, disability residence or a residential aged care facility (RACF).
What are some tips for delivering a COVID-19 vaccination safely in a patient’s home?
Who to vaccinate at home?
- You could gather the names of all of the patients to whom your doctors pay home visits. Decide as a group how you will work through the list.
- If you are a COVID-19 vaccinating clinic, you could use extra pre-drawn doses from the clinic to target homebound patients.
- If you are not, you could make an arrangement with a local COVID-19 vaccinating clinic to attend to your homebound patients.
- You might ask the patient if they have any other family members who want to be vaccinated on the day, and then run a “mini clinic”.
Transporting the vaccine
- Make sure you have a lightproof container to transport the vaccines.
- It is okay to transport pre-drawn doses if you can appropriately store the vaccine and deliver it promptly. This means protecting it from light and maintaining appropriate cold chain – that is, between 2-8°C. This also means delivering the vaccine within one hour if it is kept at room temperature, or six hours if it is stored at 2-8°C.
- If you can deliver the vaccine within one hour it is OK to not to monitor the cold chain. Just keep it cool and out of the light. This is probably the most viable option for most home visit vaccinations.
- If delivery will take longer than one hour then you will need to manage the cold chain using a mobile solution, such as an appropriate cooler with ice blocks or gel packs stored in the freezer. Ice or gel packs need to be conditioned before being used for transport and the vaccines need to be insulated from them. One of the greatest risks to vaccines is freezing during transport in a cooler. This risk increases if the ice or gel packs are not correctly conditioned. See Section 9 in the National Vaccine Storage Guidelines for more information on how to correctly cool and pack a cooler for transport, and how to use a mobile temperature monitor to monitor the temperature inside it.
Vaccination safety off site
- Have an anaphylaxis kit with adrenaline available for the vaccinator to take with them.
- The usual process of obtaining consent, assessing safety for the vaccine, a post-vaccination waiting period and uploading to the Australian Immunisation Register will still apply
How do I bill for a vaccine given in a patient’s home?
The MBS has recognised the extra time taken to vaccinate in a patient’s home, residential disability setting or RACF by introducing the COVID-19 vaccination flag-fall fee. This can be claimed once for the first patient seen at the person’s place of residence. It is co-claimed with other COVID-19 consultation items, and, like the other COVID-19 vaccination items, must be bulk billed. You could claim:
Flag-fall fee item 90005: $57.25
+
Indepth COVID-19 assessment item 10660 (if appropriate): $39.10
+
Appropriate Vaccination item (below are the in hours standard items for metropolitan areas, other items might apply):
Assessing COVID-19 vaccine suitability dose 1 item 93624: $31.05
Or
Assessing COVID-19 vaccine suitability dose 2 item 93644: $24.45
+
Any unrelated visit items
For further information
Australian Department of Health: Covid-19 vaccines advice for vaccine providers
Australian Department of Health: National Vaccine Storage Guidelines
HealthPathways Melbourne
Visit the Outreach and mobile clinics page on Health Pathways Melbourne for assistance on how to manage and coordinate off site vaccinations.
Are you a GP or health professional in our region who doesn’t have access to HealthPathways Melbourne? Request access online or contact info@healthpathwaysmelbourne.org.au






