
The Strengthening Care for Children project was undertaken by the Royal Children’s Hospital, Murdoch Children’s Research Institute and North Western Melbourne Primary Health Network (NWMPHN) between 2017–19. Five general practices in the NWMPHN region were recruited and supported to take part in this pilot study.
The study examined the impact on child health outcomes of providing greater specialist support to general practice in treating and managing paediatric patients.
Participating practices gained weekly access to an experienced Royal Children’s Hospital paediatrician for patient co-consultations, plus a monthly case conference for health professionals with the paediatrician. Practices were also able to access the paediatrician by phone and email for same-day advice.
The model was designed to support GPs to deliver higher quality care, with greater confidence, for a broader range of childhood health concerns. The pilot study measured:
- feasibility and acceptability of the model
- GP confidence in paediatric care
- GP referrals and care quality
- family experience and preference for care
- costs
Sustainability planning was completed in partnership between NWMPHN and the practices. Two practices have hired paediatricians, while others are exploring options for access to paediatric support and learning (for example: a webinar program).
The research team plans to complete a larger, multi-site trial across two states, to rigorously evaluate the effectiveness and viability of the model in high referral areas.
Neal Street Medical Clinic
Neal Street Medical Clinic in Gisborne was one of the practices involved in the project.

Practice Manager Elise Sloss explained that Neal Street Medical Clinic is a dynamic practice that prides itself on quality health care. This was echoed by Practice Partner Dr Umair Masood, who said that they chose to participate in the project as they thought it would benefit patients.
“There is a great need for paediatric specialist input in the community and we thought this was a great opportunity to nurture this,” Dr Masood said.
“We were hoping to gain more experience in dealing with the paediatric cases that we could manage in-house with reduced referrals where possible.
Elise Sloss also indicated they were hoping to increase their GPs’ confidence in treating paediatric cases:
“We hoped for greater understanding of common paediatric conditions so that the GPs felt more confident in treating and not just referring off to hospital, therefore minimising hospital admissions.”
“Through the project we learned not to just assume that the paediatrician understands how a GP clinic is run; the paediatrician gained greater awareness of general practice and the GPs gained greater understanding of how a paediatrician works.”
“We also learned that there are opportunities to reduce hospital admissions by facilitating greater awareness and understanding of common conditions for the GP. Many of the GPs lacked understanding in similar things.”
Dr Masood added:

“We will add a lot of clinical pearls from a collaboration with the paediatrician. We were also able to enhance our own skills and are now able to approach certain paediatric issues in a different way.”
“The project also identified what we are doing well and also what we need to learn more about. We have started dealing with certain complex paediatric patients within our practice and are only requesting help from specialists when required. We have found that we are referring a lot less patients to hospital outpatients.”
Elise Sloss noted that participating in the project gave the team a sense of achievement that they have been part of something so worthwhile.
Dr Masood also noted that the patients have all been very enthusiastic and supportive of the project:
“We have had nothing but praise and encouragement from the patients with regards to this project. A lot of parents did find this extremely useful and still keep asking whether the project will continue.”
How can your practice get involved?
Through this project we found that developing and embedding a GP–paediatrician integrated model of care in Australia’s primary health care system is feasible and acceptable. It improves the confidence of GPs and the quality of paediatric care, benefits families and children, and may reduce referrals to hospital services.
This integrated care model could be:
- Replicated for chronic complex care that burdens the hospital system;
- Implemented in service hubs with co-located paediatricians; and
- Extended to include telehealth for rural or regional hubs.
If you would like to find out more please contact primarycare@nwmphn.org.au
NWMPHN is also currently planning its 2019–20 education and training calendar. If you are interested in participating in one-hour case study discussions conducted by subject matter experts and delivered by webinar, please register your interest by emailing primarycare@nwmphn.org.au with your preference for:
- Topic
- Day and time
Where can I get more information?
The overall outcomes of the project are outlined in the image below.
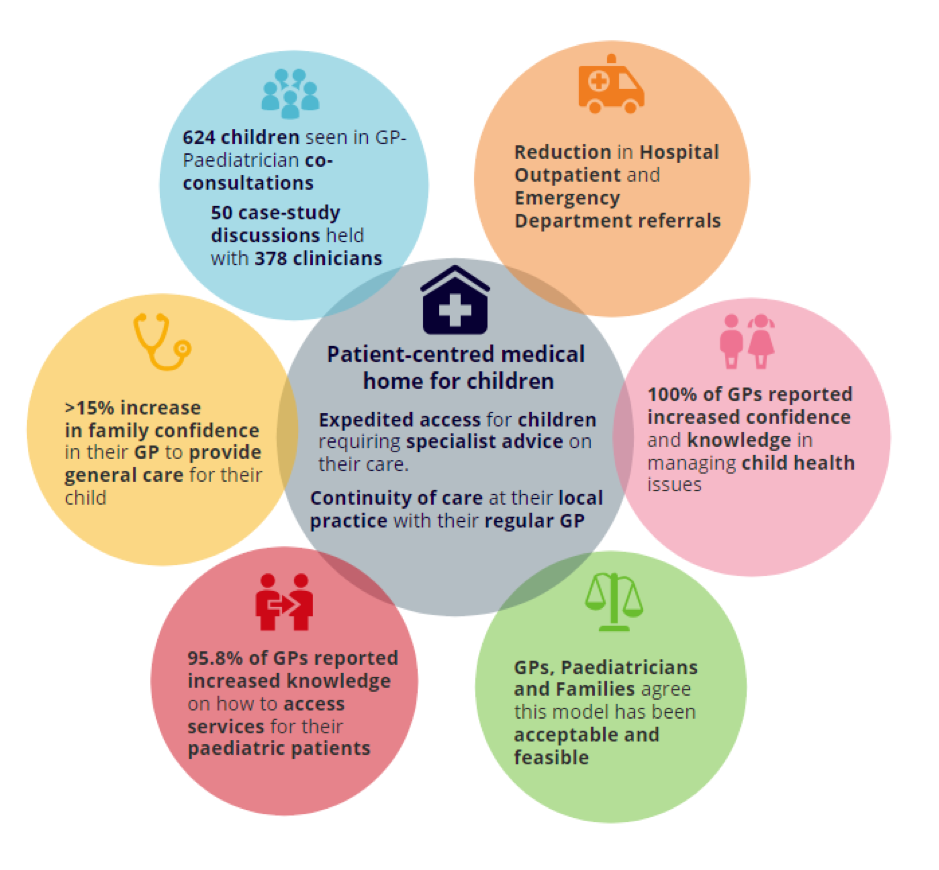
Paediatric HealthPathways
HealthPathways Melbourne is a free, web-based tool with relevant, local and evidence-based information on the assessment and management of common clinical conditions, including referral guidance, clinical and patient resources.
If you do not have access to HealthPathways please email info@healthpathwaysmelbourne.org.au.
More information about the Statewide Paediatric HealthPathways Project is available on the Victorian and Tasmanian Primary Health Network Alliance website.





