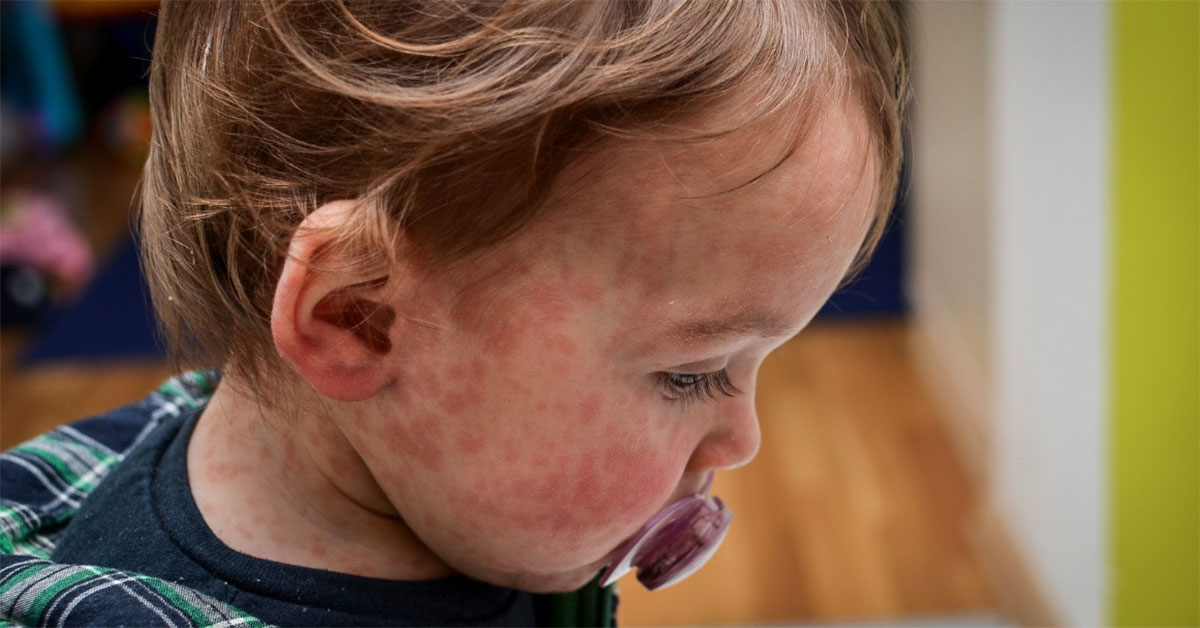
Measles vaccination rates are falling, and local transmissions continue to be recorded.
Are we on the verge of a severe outbreak?
Here are some tips for improving vaccination rates.
Why is measles vaccination so important?
Measles is a highly contagious viral illness with a relatively high rate of complications. It can be severe, often leading to hospitalisation or death. Protection from measles is available through a safe and effective vaccine.
What’s happening to vaccination rates?
The World Health Organisation declared measles eliminated in Australia in 2014.
However, vaccination rates for multiple conditions, including measles, are falling worldwide, including here. This trend started during the COVID-19 pandemic, but continues to worsen.
Experts agree that vaccination coverage of 95 per cent or greater of a two-dose measles-containing vaccine is needed to create herd immunity – defined as the level of immunisation required to protect communities and to maintain measles elimination.
Victoria’s current vaccination rate for measles in two-year-olds currently sits at 92.3 per cent, which is well below the threshold. Additionally, adults vaccinated between 1966 and 1992 may have only received one dose of the vaccine, which is insufficient for full immunity.
Currently most measles cases in Victoria have been imported from overseas with local transmission numbers small. However, with falling vaccination rates it seems only a matter of time before there is a significant local outbreak – such as the one in Texas earlier this year that resulted in two deaths and over 100 hospitalisations.
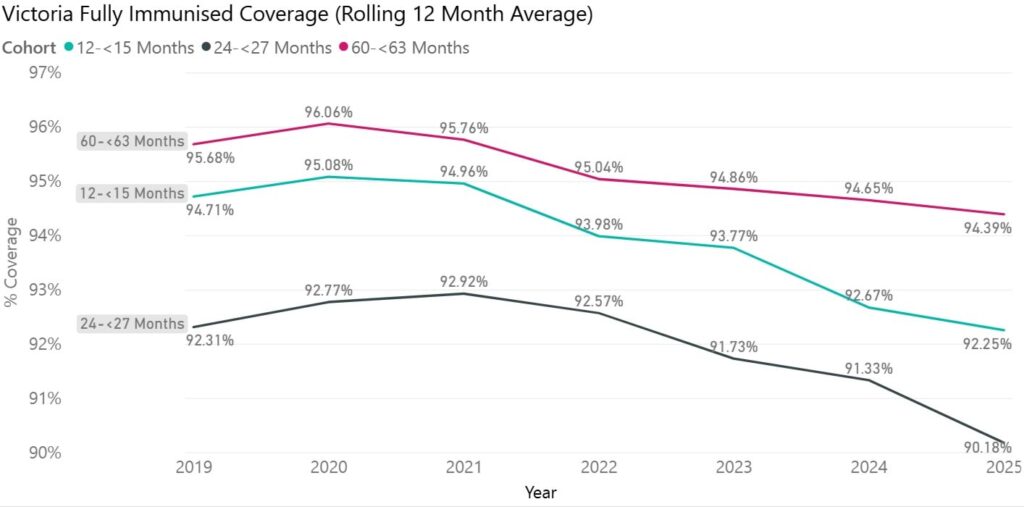
Source: Victorian Department of Health
What’s behind the reduction in measles vaccination rates?
Vaccine rates have been falling since the pandemic. A February 2025 article by Peter Breadon and Wendy Hu from the Grattan institute identified two main issues:
- Hesitancy, driven initially by misinformation around COVID-19 vaccinations, and by ongoing lack of trust in health providers.
- Access issues including cost and barriers to getting appointments, underpinned by the cost-of-living crisis.
What can general practices do to improve measles (and overall) vaccination rates?
There are several avenues and options available to general practices for boosting numbers. They fall roughly into three areas.
Improving systems
- Assign an immunisation champion. Designate a staff member to lead immunisation efforts, monitor coverage, and coordinate recalls and education.
- Use AIR reports to identify groups that are un or under vaccinated. AIR reports are more comprehensive than other records because they include vaccines given elsewhere.
- Use health record prompts. Create recalls or alerts in the electronic health records to flag patients identified in AIR report as due or overdue for vaccines.
- Leverage digital tools such as POLAR for targeted immunisation reports
- Use reminder and recall systems by sending SMS, letters, or phone calls to alert patients to upcoming or missed vaccinations.
Improving access
- Extend clinic hours. Offer after-hours and weekend vaccination clinics to improve accessibility for working families and busy individuals.
- Offer different types of appointments, such as drop-ins and nurse-led vaccination clinics.
- Opportunistic vaccinations. Check immunisation status during any patient visit and offer vaccines when due, even if the visit is for another reason.
- Standing orders. Implement standing orders allowing nurses to administer vaccines without direct GP involvement.
- Co-administration of vaccines. Where safe, offer multiple vaccines in one visit to reduce missed opportunities.
Addressing the vaccine hesitant
- Strong GP recommendations are among the most influential factors in decision-making.
- Provide clear endorsement of the vaccine’s safety and importance.
- Staff training. Regularly train staff on current immunisation schedules and effective communication strategies, especially for vaccine-hesitant patients.
- Avoid confrontation and acknowledge concerns respectfully.
- Use motivational interviewing techniques. Ask open-ended questions, affirm concerns, and provide information.
- Address specific concerns and misinformation, for instance regarding side-effects, or timing.
- Provide written material, such as fact sheets from NCIRS , Melbourne Vaccine Information Centre or the Questions about vaccination booklet.
Language matters
- Frame recommendations positively, such as “this vaccine is the best way to protect your child from serious illness.”
- Normalise vaccination by saying “most of my patients choose to get this vaccine.”
- Say “I’ve had this vaccine myself,” or “I recommend this for my own family.”
- Culturally sensitive communication is vital. Use tailored messaging and community engagement to reach underserved or hesitant populations, such as multicultural or First Nations communities.
Who is eligible for a free measles (MMR) vaccination?
A two-dose course of a measles-containing vaccine is available free under the National Immunisation Program for:
- children aged 12 months and over
- all people (including refugees and humanitarian entrants) aged less than 20 years who did not receive the MMR/MMRV vaccines in childhood
- refugees and humanitarian entrants aged 20 years and over.
Additionally, all states and territories fund a dose of MMR vaccine for:
- children aged six months to less than 12 months* who are travelling to a country where measles is endemic, or outbreaks are occurring. (If an infant receives a dose of MMR vaccine between six and 11 months of age, they still need to receive thetwo2 recommended vaccine doses at 12 and 18 months.)
- adults born during or after 1966.
Victorian Enhanced Measles Response Program
In response to increased cases of measles and local transmission, the Victorian Department of Health has launched the Enhanced Measles Response Program. The goal of this program is to increase the MMR coverage of adults.
The program gives providers access to free MMR vaccines for adults aged 20-59 who:
- were born during or after 1966 without two documented does of measles containing vaccine
- are unsure of vaccination status.
The program is being delivered via Local Public Health Units, please see their websites for further details:
For more information
- Immunisation pathways | HealthPathways Melbourne
- Measles pathway | HealthPathways Melbourne
- Vaccination coverage rates for Victoria | Victorian Department of Health





